An estimated 10% of the world’s population is affected by chronic pain. Finding effective, long-lasting and drug-free pain relief can be a huge challenge.
However, there is a growing body of evidence demonstrating that Transcutaneous Electrical Nerve Stimulation (TENS) therapy may be the answer.
What is TENS therapy?
Transcutaneous electrical nerve stimulation (TENS) therapy is the most widely used type of electrotherapy for the management of both chronic and acute pain.
The therapy is administered through a TENS unit (a small battery-operated device) that has leads connected to sticky pads (electrodes), although wireless versions are becoming increasingly popular.
A mild electrical current is sent from the device to the pads, providing a drug-free treatment option for a number of conditions including back pain and labor pains.
Can TENS therapy provide pain relief?
Physicians and other healthcare professionals have been using TENS as a form of pain relief since the 1960s.
While there is conflicting information on the impact of TENS, there is a growing body of significant research that shows how powerful TENS can be for pain relief.
One of the biggest advantages is the fact that it’s a drug-free way to relieve pain.
TENS therapy is therefore ideal for those who can’t take prescribed pain medication, or choose not to due to the side effects.

Pin it for later!
Don’t forget to pin this article about TENS therapy for later!
TENS is typically used in combination with other treatments to help manage pain.
Though not a cure, it can help you treat the root cause of the problem.
A fishy fact:
In 2500 BC stone carvings depicting Roman physicians using electric fish to treat conditions were discovered.[1]
Confused About The Difference Between TENS And EMS?
Many people confuse TENS with electrical muscle stimulation (EMS). While TENS and EMS units can look almost identical, the two have completely different purposes so it’s imperative that you choose the correct type of device.
A TENS unit is designed to stimulate the nerves to help reduce both chronic and acute pain. However an EMS machine makes the muscles contract.
EMS therefore is more commonly used for muscle building, recovery, training, rehabilitation, injury prevention and cosmetic appearance.
What’s the cost of TENS therapy?
The initial cost involves the purchase of the machine, which typically includes the device, lead wires, pads (electrodes), and the first set of batteries or a charger (if it’s rechargeable, like most modern devices tend to be).
Over the counter (OTC) TENS machines can be found for as little as $20 – and in some cases – perhaps even less.
More expensive devices can cost hundreds and even thousands of dollars.
However price doesn’t always equate to performance so it’s worth reading a few TENS unit reviews before making a purchase.
In terms of maintenance, pads need replacing after a certain number of uses or when they wear out, and of course non-rechargeable devices need replacement batteries.
Do you need a prescription to try TENS therapy?
Even though TENS machines can be purchased without a prescription (in many countries, like the USA, Canada, and UK), there are a few individuals who should not use them.
For this reason, it is best to first seek the advice of a medical professional (e.g. a doctor, physical therapist or chiropractor).
Medical sources and TENS manufacturers tend to list similar warnings about who should not use the devices.
However, they are very rarely identical, which is why you should always speak to a health professional.
As an example, the NHS website (the UK’s National Health Service) states that people with a pacemaker (or any other type of electrical or metal implant in their body) should seek medical advice before using a TENS unit.
It says the same for anyone who is pregnant, has epilepsy or a heart rhythm disorder.
Certain TENS manufacturers also advise that anyone who has recently undergone a surgical procedure, or has cancer or any other health condition should not use the unit without speaking to a physician.
So if you’re in any doubt about suitability it’s certainly worth checking before you begin.
Does TENS therapy have any side effects?
Most people who use TENS do so without experiencing any side effects.
However, in the past it was common that a very small number of users may have an allergic skin reaction to the pads (approximately 2-3%).
To counter this, manufacturers have moved to special latex-free pads. If you do have allergies, you should still always check the material of the pads before use.
Other side effects from a TENS unit are often down to people not following the guidance and overusing the device or having the intensity set too high.
Using the machine too much can make the area being treated sore.
While using excessive intensity can make muscles twitch and result in unpleasant sensations.
If you use the machine as advised by your physician and the manufacturer, it’s unlikely you’ll experience any side effects.
FAQs
What does a TENS unit feel like?
How many channels and pads do I need?
What is the difference between programs and modes?
Should I buy a rechargeable device?
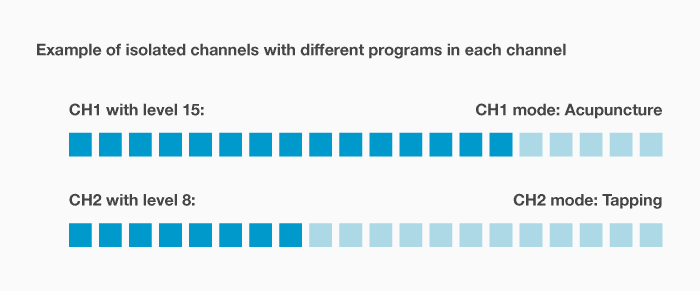
Do I need independent intensity controls for each channel?
What are fully isolated channels?
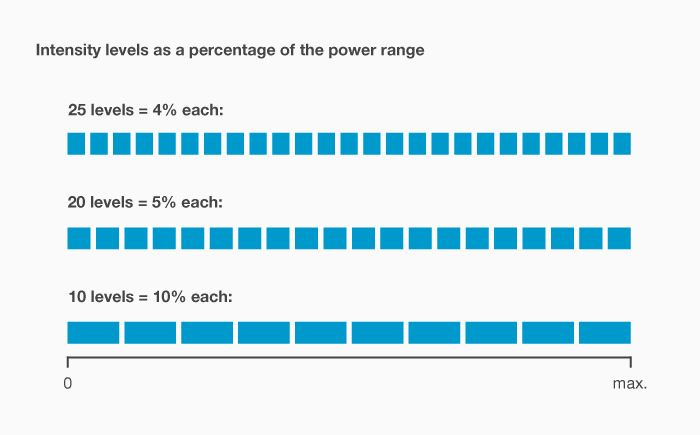
Do more intensity levels mean more power?
Is it better to have more intensity levels?
What conditions can a TENS machine be used for?
How do I find out more about TENS units?
References
- NuroKor (2019). How long have we been using electricity for therapeutic purposes? [Online]. Available from: https://nurokor.co.uk/blogs/videos/how-long-have-we-been-using-electricity-for-therapeutic-purposes [Accessed 2 February 2023]. ↩